Understanding and Living with Osteoporosis
by Stefanie Zinchiak M.Ed.
Medically Reviewed by Dr. Linda Lemay M.D.

Understanding Osteoporosis
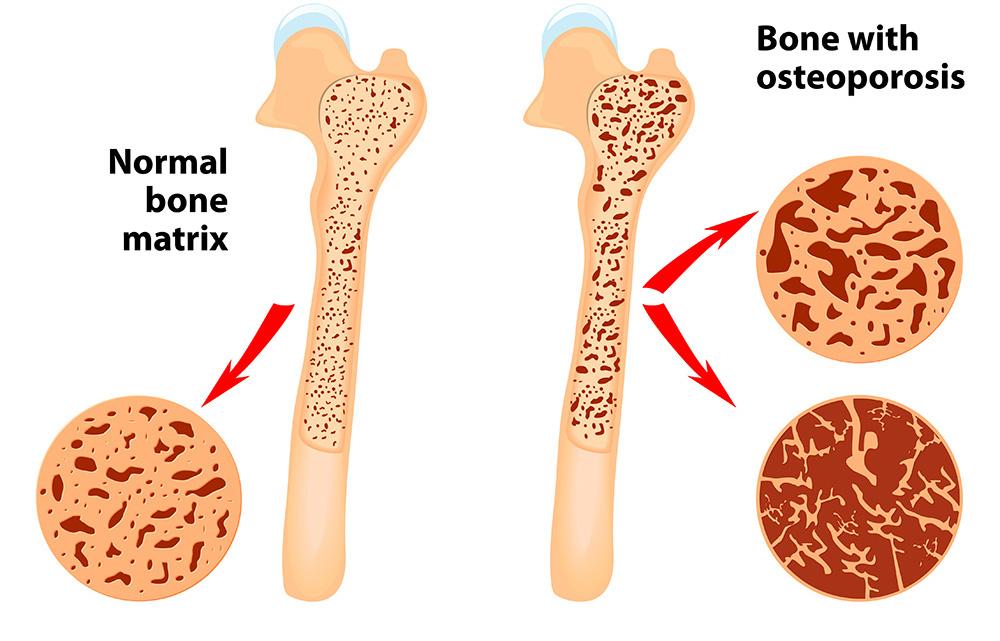
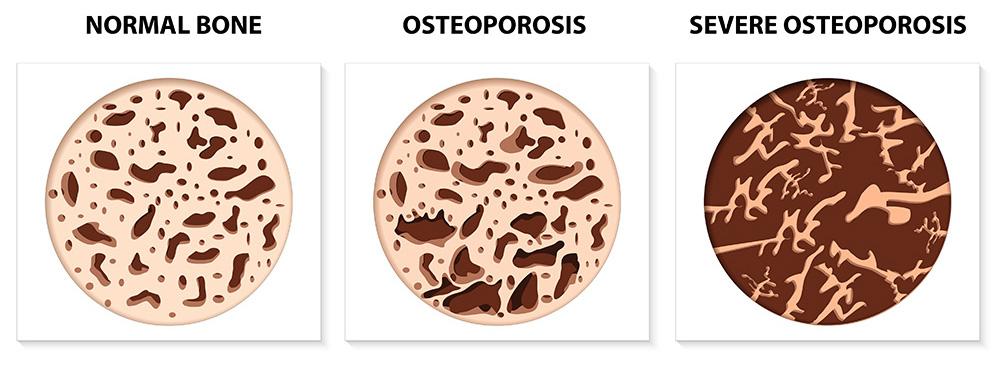
Osteoporosis is a progressive disease of the bones that is caused by a loss of bone mass. This loss of bone mass causes the bones to become weak and more likely to break or fracture. The term osteoporosis means porous bone, and when looking under a microscope, a healthy bone will look spongy, having spaces and holes throughout the bone tissue. With osteoporosis, the ‘holes’ are much bigger, which indicates a loss in bone mass, or density. This results in weaker bones that break and fracture easily.
While falling is a common cause for breaking bones, in severe cases, bones can break just from bumping into furniture or sneezing. Breaking a bone can cause severe pain and disability, and can impact your ability to perform normal daily tasks. Common locations where fractures may occur include the hip, spine, wrist, arms and legs. Unfortunately, many individuals are not even aware that they have the disease until a bone has fractured, or it becomes noticeable that the person is getting shorter or that their upper back is curving forward.
If you’re in search of an orthopedic surgeon, check out the Women’s Choice Award America’s Best Hospitals for Orthopedics to be sure you’re getting the best treatment in your community.
Did You Know?
According to the Bone Health & Osteoporosis Foundation, approximately 1 in 2 women and up to 1 in 4 men age 50 and older will break a bone due to osteoporosis.
Risk Factors & Prevention
Some of the risk factors for developing osteoporosis are out of your control. These include being female, getting older, having a small body frame, having a family history of osteoporosis, and the usage of some medications, such as steroids or cancer treatments.
Risk factors and causes that are in your control include getting enough exercise, not smoking or drinking alcohol excessively, avoiding excessive usage of certain medications, and having an adequate daily intake of calcium and vitamin D. Weight bearing aerobic exercises in which your bones must support your weight help slow mineral loss in your bones. Examples of weight bearing exercise for osteoporosis include walking, dancing, low-impact aerobics, stair climbing, gardening, etc. While swimming and cycling are great for overall health, they do not provide the weight-bearing load needed to keep your bones strong.
Individuals should also take note of the warning signs for osteoporosis, which include a loss in height, developing a hunched back or posture, or if you’re over 45 years of age and have broken a bone.
For individuals looking to prevent the disease or slow its progression, it’s critical to maintain an adequate daily intake of calcium and vitamin D, and exercise regularly. There is also some evidence that certain yoga poses can help prevent osteoporosis, especially those involving balancing on one leg at a time.
Diagnosis
Your healthcare provider will first assess your condition by looking at your medical history and giving you a physical exam. Diagnosis of osteoporosis can be done with a simple, painless test that measures bone density. One common test is called a dual-energy X-ray absorptiometry, or DXA. This test takes an X-ray of your bones, which then tells you how strong or weak your bones are, and can predict your risk for a bone fracture.
Treatment Options
If you suffer with osteoporosis, your treatment plan will likely include a combination of a calcium-rich diet, adequate intake of vitamin D, regular exercise, and medication therapies. Medications that have been approved for the treatment or prevention of this disease, include the following:
- Bisphosphonates: these FDA approved drugs can slow the rate of bone loss, can help increases bone mass, and can decrease the risk of fractures.
- Calcitonin: this hormone medication can decrease the rate of bone loss, help prevent spine fractures, and also provide pain relief.
- Selective Estrogen Receptor Modulators (SERMs): this hormone medication can decrease the rate of bone loss and help prevent spine fractures in postmenopausal women.
- Hormone (or Estrogen) Replacement Therapy: this helps prevent bone loss and reduce the risk of bone fractures. However, there are other health risks associated with these medications, so risks and benefits should be discussed with your doctor.
- Teriparatide: a form of human parathyroid hormone, which helps the body build up new bone.
Recommended Daily Calcium and Vitamin D Intake: (From the Institute of Medicine)
|
Age & Gender |
Calcium (mg/day) |
Vitamin D (IU/day) |
|
9 – 18 years old |
1,300 |
600 |
|
19-50 years old |
1,000 |
600 |
|
19-50 years old, pregnant/lactating |
1,300 |
600 |
|
51-70 years old, males |
1,000 |
600 |
|
51-70 years old, females |
1,200 |
600 |
|
71+ years |
1,200 |
800 |
Living with Osteoporosis
The most serious risk of having osteoporosis is a bone fracture, so it’s important to modify your home and daily activities to prevent falls and fractures.
- Wear shoes with rubber soles for more traction
- Use hand rails whenever possible
- Use a cane or walker, if needed
- Keep hands free by wearing a shoulder bag, fanny pack or backpack purse
- Be cautious on curbs, inclines, and stairs
- Be careful on marble or tile surfaces and stay on carpet runners whenever possible, especially on wet surfaces or on rainy days
- Keep hallways and entrances lit when it’s dark
- Remove throw rugs, and rearrange fall hazards like loose wires and cords around your home
- Make sure carpets are skid-proof, and use non-skid rubber mats in the shower or tub
- If you have to use a stepstool, make sure it’s sturdy and has handrails and wide steps
- Use assistive devices, such as grasping devices to avoid straining or injuring yourself from excessive bending or reaching
- Get help with carrying or lifting anything heavy
Where to Go
According to a study reported in The Journal of the American Academy of Orthopaedic Surgeons, structural anatomy differences, hormones, and genetics are factors in optimizing care for male vs. female orthopedic patients. “Women have different orthopedics needs, particularly as they grow older and become more at risk for osteoporosis and fractures. Being treated with the proper level of care impacts one’s health, well-being, and healing, so it is critical for women to know those hospitals that have demonstrated the highest level of quality care for their patients, with a special focus on the needs and preferences of women. said Delia Passi, founder and CEO of the Women’s Choice Award. If you’re in search of an orthopedic surgeon, the Women’s Choice Award America’s Best Hospitals for Orthopedics have met the highest standards for orthopedics across the U.S.
Questions to Ask Your Doctor:
Q: How can I prevent or slow the progression of this disease?
Q: What can I do to avoid injuries? Where can I find assistive devices and what do you recommend?
Q: What is my treatment plan? (How much daily calcium and vitamin D do you recommend for me? What do you suggest for exercise? What medication will I be on and why?)
Resources:
America’s Best Hospitals for Orthopedics
Bone Health & Osteoporosis Foundation
National Osteoporosis Foundation
National Institutes of Health
American College of Rheumatology
Know Where to Go, Know What to Do
This content is for informational purposes only and is not intended to provide medical advice or to treat, diagnose, cure or prevent any disease or condition. Always seek the advice of your healthcare provider.
Sources:
https://www.nlm.nih.gov/medlineplus/osteoporosis.html
http://www.womenshealth.gov/publications/our-publications/fact-sheet/osteoporosis.html#a
http://nof.org/articles/7
http://orthoinfo.aaos.org/topic.cfm?topic=a00232